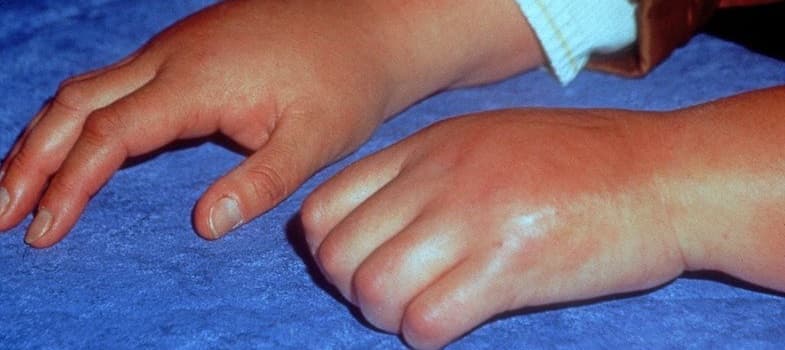
What is Complex Regional Pain Syndrome?
Complex Regional Pain Syndrome (CRPS), also known as Reflex Sympathetic Dystrophy (RSD), is a condition involving chronic, intense pain that usually occurs in the arms, hands, legs or feet. It is thought that CRPS is precipitated by trauma to nerves in the affected area. CRPS is normally seen in middle-aged people, but has been reported to occur in younger individuals.
There are two types of CRPS. CRPS 1 is a chronic nerve disorder that occurs in an extremity (e.g., arm, leg, hand, foot) after a minor injury. CRPS 2 is caused by direct injury to a nerve.
Complex Regional Pain Syndrome Causes
The cause of Complex Regional Pain Syndrome is not fully understood, and there is still no cure. One theory is that CRPS is caused by the sympathetic nervous system. This theory postulates damage to the nervous system, particularly in nerves that control blood vessels and sweat glands, is responsible for the appearance of CRPS symptoms. Car accidents, penetrating wounds, crush injuries, surgery, infection, and fractures are examples of severe traumas that may cause direct injury to a nerve and lead to development of CRPS. Damaged nerves involved in CRPS may lose the ability to govern blood flow, sensation, and temperature in the affected areas. This may cause chronic pain and other problems in local tissues.
An alternate theory that CRPS is caused by an inappropriate immune response is evidenced by the appearance of redness, warmth, and swelling in affected areas. These signs are associated with inflammation, a characteristic component of an immune response.
The signs and symptoms of CRPS may worsen over time, or spontaneously resolve. The main symptom of CRPS is intense, continuous, burning pain that usually occurs in the extremities. Often, the pain may begin at the site of a traumatic injury but spread throughout an entire limb. Eventually, the pain may migrate to the opposite side of the body.
The pain of CRPS can be provoked by stimuli that are not usually painful, such as the touch of a feather on the skin (allodynia). In addition, a normally painful stimulus may cause disproportionately severe irritation and pain (hyperalgesia).
The allodynia and hyperalgesia of Complex Regional Pain Syndrome are indicators of central sensitization. In this condition, local tissue injury and inflammation activate the peripheral nervous system (PNS), which sends signals to the central nervous system (CNS). The excitability of neurons within the CNS increases, causing normal inputs from the PNS to produce abnormal responses. Low-threshold sensory fibers activated by light touch excite neurons in the spinal cord that would normally respond to more painful stimuli. As a result, a light touch that would normally produce a harmless sensation now produces significant pain.
Additional Symptoms
In addition to pain, Complex Regional Pain Syndrome patients may also experience:
- Changes in skin color (e.g., blotchy, purple, pale, red)
- Changes in skin texture (e.g., shinier, thinner, sweatier)
- Changes in skin temperature (e.g., affected area is warmer or cooler than surrounding tissues)
- Increased skin sensitivity
- Changes in hair and nail growth patterns
- Muscle atrophy
- Stiffness and swelling in affected joints
- Reduced range of motion in the affected extremity
- Depression and anxiety, since the pain and other consequences of CRPS can be severe and long-term
Many experts believe CRPS progresses in three stages, although this progression has not been confirmed by clinical studies. These stages include1:
Stage 1 (1-3 months)
- Changes in skin temperature, alternating between warm and cold
- Faster growth of nails and hair
- Muscle spasms
- Joint pain
- Severe burning, aching pain that worsens with the slightest touch or breeze
- Skin becomes blotchy, purple, pale, or red; thin and shiny; swollen
Stage 2 (3-6 months)
- Continued changes in skin
- Nails crack and break more easily
- Pain becomes worse
- Hair growth slows
- Stiff joints and weak muscles
Stage 3
- Irreversible changes can be seen
- Limited movement in limb because of tightened muscles and tendons (contracture)
- Muscle wasting
- Pain in the entire limb

Diagnosing and Treating CRPS
In order to diagnose Complex Regional Pain Syndrome, other conditions must be ruled out. The doctor will take a medical history and perform a physical exam that includes evaluation of the patient’s pain, range of motion, and sensory function. Blood testing may be performed to rule out other inflammatory or rheumatologic conditions. Nerve conduction studies may be ordered to eliminate clinical suspicion of peripheral neuropathy, or nerve entrapment conditions. Magnetic resonance imaging (MRI), CT scan or X-ray may be performed to rule out any soft tissue causes for the patient’s neuropathic symptoms. When the possibility of all other conditions has been eliminated, the doctor may diagnose a patient with CRPS.
Early diagnosis of CRPS is important. Although the progression of the disease cannot be stopped, it can be slowed, and the patient’s quality of life can be boosted with an appropriate treatment program. Since there is no cure for CRPS, treatment focuses on slowing the progression of the disease and managing pain and other symptoms. Some of the diverse and effective treatment options include:
- Pharmacotherapy – Certain medications may help mitigate the symptoms of CRPS. Pain medicines such as non-steroidal anti-inflammatory drugs (NSAIDs and other analgesics may alleviate pain. Corticosteroids, medications to inhibit bone loss, membrane stabilizing drugs and antidepressants may also be effective. A controlled randomized clinical trial found intravenous magnesium significantly improved pain, impairment and quality of life and was well tolerated in CRPS type I patients2; intravenous ketamine was found to have similar benefits in CRPS 1 patients in a different study3.
- Physical and Occupational Therapy – These therapies should be started as early as possible. Certain exercises can help preserve range of motion and functionality of joints and muscles in CRPS patients.
- Intrathecal Pump Implants – Implanted pain pumps can be extremely helpful in providing long-term pain control. A study examining the efficacy of intrathecal therapy in people suffering pain due to cancer showed pain reduction in 66.7% of patients4.
- Cognitive Behavioral Therapy (CBT) – Based on the idea that certain thought and behavior patterns can influence the course of illness, CBT teaches psychological, physical and social strategies to help patients cope with pain.
- Spinal Cord Stimulation (SCS) – An implanted electrical device decreases the perception of pain by confusing the spinal cord and pain processing centers of the brain. Initially, a trial is conducted to determine whether the device will help the patient on a long-term basis. It is effective in about 50–70% of patients5.
- Peripheral Nerve Stimulation – This method involves placement of tiny electrodes near the affected nerves. The electrodes release a small electrical current that inhibits pain transmission and provides pain relief.
- Epidural Steroid Injections (ESIs) – Frequently, ESIs are used for CRPS and other pain syndromes. The doctor injects a steroid into the epidural space of the spinal cord, where the irritated nerve roots are located. The medicine then spreads to other levels and portions of the spine, reducing inflammation and irritation.
- Sympathetic Nerve Blocks – A small, fine needle is inserted through the skin to block sympathetic nerves responsible for excessive pain. Procedures that target the face and upper extremities include the Stellate Ganglion Block and Brachial Plexus Nerve Block. For the lower extremities, Lumbar Sympathetic Nerve Blocks are commonly performed.
- Infusions Techniques – A small catheter is inserted through a needle into the epidural space or directly next to affected nerves. Local anesthetic and other medications are administered through the catheter over extended periods. Pain relief can be substantial and long-lasting when the nerves are blocked continuously with an infusion.
- Biofeedback – This therapy teaches awareness of processes normally thought to be involuntary inside of the body such as blood pressure, temperature and heart rate, enabling some degree of conscious control of these processes. Biofeedback can influence and improve level of pain and promotes relaxation.
- Support Groups – Living with the pain of CRPS can be difficult. Support groups can help CRPS patients cope with the difficulties and discomforts of living with their chronic condition.
The prognosis for Complex Regional Pain Syndrome is variable. However, outcome is generally improved with early diagnosis and treatment. Sometimes, if the condition is caught within the first stage, restored range of motion and even remission are possible. Without early diagnosis and treatment, changes to tissues will eventually become irreversible. Patients who live with CRPS and other painful conditions are encouraged to seek help as soon as possible to prevent long-term damage that cannot be reversed.
Wake Spine & Pain Specialists understands the burden of living with pain and strives to help patients regain their quality of life. Our caring practitioners are dedicated to working closely with patients to create tailored individual pain management programs designed to restore good health and happiness. To investigate treatment options for your CRPS, call to schedule an appointment with us today.
References
- Hoch, DB, & Zieve, D. National Institutes of Health, Medline. (2011). Complex regional pain syndrome U. S. Library of Medicine: Retrieved from www.nlm.nih.gov/medlineplus/ency
- Collins S, Zuurmond WW, de Lange JJ, van Hilten BJ, & Perez RS. (2009). Intravenous magnesium for complex regional pain syndrome type 1 (CRPS 1) patients: a pilot study. Pain Med., 10(5), 930-40.
- Sigtermans MJ, van Hilten JJ, Bauer MC, Arbous MS, Marinus J, Sarton EY, & Dahan A. (2009). Ketamine produces effective and long-term pain relief in patients with Complex Regional Pain Syndrome Type 1. Pain., 145(3), 304-11.
- Becker, R, Jakob, D, Uhle, L, Riegel, T, & Bertalanffy , L. (2000). The significance of intrathecal opioid therapy for the treatment of neuropathic cancer pain conditions. Stereotact Funct Neurosurg., 75(1), 16-26.
- Kunnumpurath S. (2009). Spinal cord stimulation: Principles of past, present and future practice: A review. Journal of Clinical Monitoring and Computing, 23, 333-339.