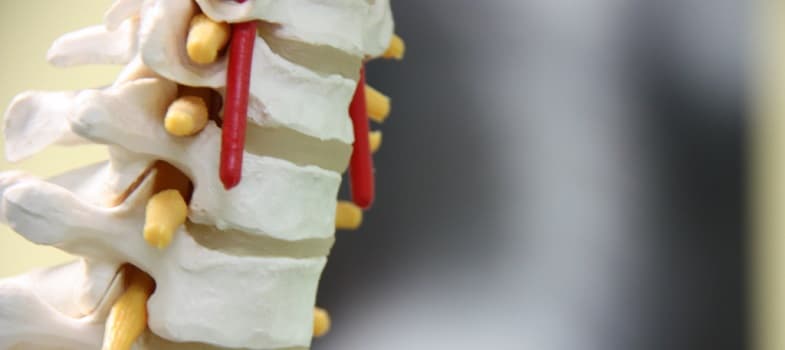
What Is Spondylolisthesis?
Spondylolisthesis is a condition in which a vertebra is dislocated and tilted forward. A vertebra is a bone of the spine, 33 of which make up the human spine. This structure acts to give support and stability to most of the body, make upright movement possible, and to protect the spinal cord, a thick length of neural tissue that extends from the brain to the pelvis. Vertebral displacement can have significant effects on gait, balance, and the integrity of the spinal cord. In the two most common forms of spondylolisthesis, this occurs gradually over time, resulting in progressive, chronic discomfort rather than acute pain.
Spondylolisthesis is most often seen in the vertebrae of the lower back (in which forward displacement may be apparent due to characteristic posture defects) but can also occur in the spinal bones of the neck, which may pose a more immediate danger to the health of people affected.
This condition may cause a general, low to moderate level of back pain (depending on which vertebrae are affected) in its own right, but may also contribute to other spinal abnormalities, which are associated with chronic back or leg pain that may be severe. These include spinal stenosis, in which vertebrae collapse or are displaced to the point that they impinge on the spinal cord, compressing it and causing pain or other neurological complications.
Spondylolisthesis may also contribute to vertebral fractures, which are mostly seen in people over 55. This may also cause spinal cord damage, and thus chronic pain. This condition is also linked to an increased risk of scoliosis, a severe structural abnormality of the spine, in which it appears to curve to the side. Spondylolisthesis is associated with detriments to life quality, functional status, psychiatric health, and general health.
Causes Of Spondylolisthesis
One form of spondylolisthesis is isthmic spondylolisthesis, which occurs after acquiring a fracture in early life. Fractures may be the result of accidents, falls, or high-impact recreational activities such as diving or skiing. This results in a forward dislocation of a vertebra (even after the fracture heals) that may have ramifications such as chronic pain or discomfort, changes in walking and posture, and stiffness or numbness.
Degenerative spondylolisthesis is mostly associated with advancing age, and is often a result of decreases in the bone density of the affected vertebra, resulting in forward slipping. This type of spondylolisthesis may be associated with arthritis in the joints between vertebrae, or osteoporosis, a progressive degeneration of bone tissue associated with advancing age.
Treatments For Spondylolisthesis
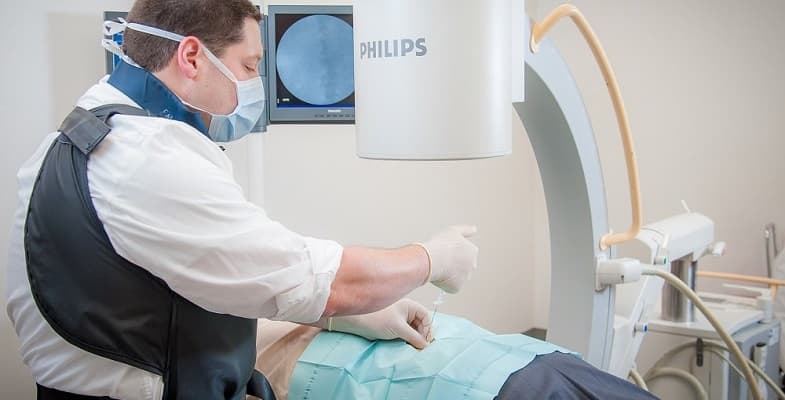
If spondylolisthesis is in an area of the spine that does not pose a threat to life, or result in severe chronic pain, its symptoms may be managed with alternative pain management strategies. An example of one of these pain management options is epidural steroid injections. These are doses of steroid medications administered directly via needle into the space between the spinal cord and a vertebra. Steroids are drugs associated with significant pain relief and the reduction of inflammation, which is a contributing factor in many chronic pain conditions.
The best form of epidural steroid injection may be a transforaminal steroid injection. The intervertebral foramen is an opening shared by a pair of vertebrae that allow nerve roots to pass between them. This is viewed as a viable alternative to back surgery in candidates who can function without it. Transforaminal steroid injection is associated with effective pain relief in patients with spondylolisthesis. However, this form of epidural injection is associated with higher risks of damage to the membrane around the spinal cord, which may result in numbness, discomfort, or other symptoms.
Muscle relaxants—oral medications with properties that contribute to the release of tension from muscles that are damaged or under stress due to spinal abnormalities—are another treatment option that have been associated with positive effects in some cases of spondylolisthesis. These drugs are also recommended for the early effects of isthmic spondylolisthesis, which may include acute pain.
Another option for very severe pain resulting from spinal displacement may be opioid medications. These are powerful painkilling drugs that inhibit the pain response of the central nervous system. Opioids are associated with considerable risks, however. These include dependence, addiction, and side effects such as organ failure. If it appears that opioid therapy may be necessary for a case of spondylolisthesis (or other conditions such as stenosis or fracture resulting from vertebral displacement), your physician and pain specialist may discuss it thoroughly in consultations, including the risks and the steps needed for responsible and safe use of these drugs.
If spondylolisthesis results in vertebral fracture (or a “collapse”), a vertebroplasty or minimally invasive procedure to restore the structure of the spinal bone using surgical bone cement may be performed. There are two main types of this: a traditional vertebroplasty or kyphoplasty. In these procedures, small, medical-grade plastic balloons are inserted through probes to support the bone while cement is injected. These procedures may be performed as a stand-alone treatment, or in combination with nerve blocks. Nerve blocks are procedures similar to epidural steroid injections, but involve administering local anesthetics in addition to steroids. These injections may also be applied to the stressed joints between vertebrae affected by displacement, which is also associated with effective pain relief.
Conclusion
Spondylolisthesis is a condition in which vertebrae are dislocated, or slip forward. This may result in a range of effects, from stiffness in the back to chronic pain. Spondylolisthesis may also contribute to other spinal conditions, such as scoliosis or vertebral fractures. Unless the nature or location of the displacement requires surgery, spondylolisthesis may be managed with pain-relieving interventions such as epidural steroid blocks or oral painkillers.
References
- Choi H-J, Park J-Y, Chin D-K, Kim K-S, Cho Y-E, Kuh S-U. Anatomical parameters of fifth lumbar vertebra in L5-S1 spondylolytic spondylolisthesis from a surgical point of view. Eur Spine J. 2014;23(9):1896-1902.
- Gille O, Challier V, Parent H, et al. Degenerative lumbar spondylolisthesis. Cohort of 670 patients, and proposal of a new classification. Orthop Traumatol Surg Res.
- Ramieri A, Domenicucci M, Cellocco P, Lenzi J, Dugoni DE, Costanzo G. Traumatic spondylolisthesis and spondyloptosis of the subaxial cervical spine without neurological deficits: closed re-alignment, surgical options and literature review. Eur Spine J.
- Srivastava A, Bayley E, Boszczyk BM. The management of high-grade spondylolisthesis and co-existent late-onset idiopathic scoliosis. Eur Spine J.
- Parker SL, Godil SS, Mendenhall SK, Zuckerman SL, Shau DN, McGirt MJ. Two-year comprehensive medical management of degenerative lumbar spine disease (lumbar spondylolisthesis, stenosis, or disc herniation): a value analysis of cost, pain, disability, and quality of life: clinical article. J Neurosurg Spine. 2014;21(2):143-149.
- O’Brien MF. Low-grade isthmic/lytic spondylolisthesis in adults. Instr Course Lect. 2003;52:511-524.
- Weinstein JN, Lurie JD, Tosteson TD, et al. Surgical versus nonsurgical treatment for lumbar degenerative spondylolisthesis. N Engl J Med. 2007;356(22):2257-2270.
- Singh K, Heller JG, Samartzis D, et al. Open vertebral cement augmentation combined with lumbar decompression for the operative management of thoracolumbar stenosis secondary to osteoporotic burst fractures. J Spinal Disord Tech. 2005;18(5):413-419.