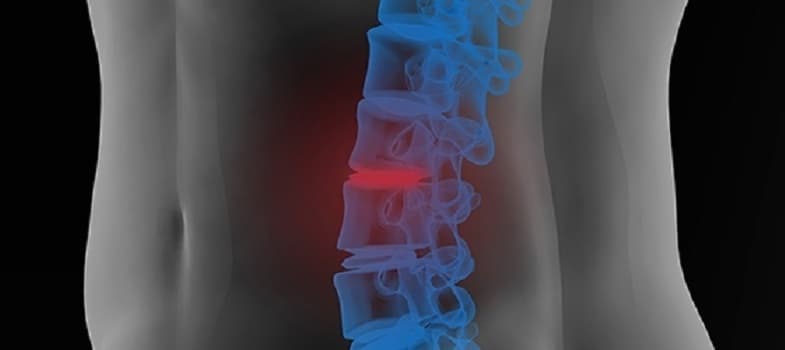
What Is Spondylosis?
Spondylosis is a term for the degeneration of spinal bones. The condition may occur in any location of the spine, but it is rarely life-threatening unless certain areas of the neck are affected. It is associated with chronic pain, which may differ in terms of severity from patient to patient. The risk of pain is increased if spinal degeneration persists in a manner or location that result in impingement on or damage to the spinal cord, or the nerves leading out of it into the body.
This could lead to another condition known as spinal stenosis, in which the spinal cord is compressed, resulting (again) in chronic pain. Stenosis may also result in leg pain, numbness, or loss of motor control. Spondylosis is also associated with the increased risk of a condition called cervical myelopathy, another form of spinal cord progression that presents with physiological hallmarks similar to those of traumatic injury.
Causes Of Spondylosis
Spondylosis is often associated with arthritis of the joints between vertebrae (the bones of the spine); however, spondylosis quite often occurs as a result of simple, age-related wear and tear that causes the degeneration of spinal structures over time, whether it be the intervertebral discs or the facet joints. Some research indicates that the presence of an existing abnormality in the thoracic or lumbar spine may increase the risk of cervical (neck) spondylosis development.
Treatments For Spondylosis
The first line of treatment for back pain, including pain caused by spondylosis, is often over-the-counter painkillers. These include non-steroidal anti-inflammatory drugs, such as ibuprofen, or muscle relaxants. Anti-inflammatory drugs may be effective in cases resulting from spinal joint arthritis. However, long-term use of such drugs is associated with an increased risk of adverse effects such as skin, gastrointestinal, or organ damage.
If painkillers prove to be ineffective, patients may consider options that elicit more effective, durable results, but are slightly more invasive. An example of these is epidural steroid injections, an administration of steroids to spinal nerves via a needle or catheter. Steroids are associated with the significant reduction of inflammation, and may therefore be most effective in cases of arthritic spondylosis. Epidural steroid injections are delivered into the space between the spinal cord and bones of the spine where they act on nervous tissue to provide medium-term pain relief.
Nerve blocks are similar to steroid injections, in that they deliver a combination of steroids and local anesthetics to spinal nerves to elicit pain relief. These formulations can also be injected into the joints between vertebrae, also known as facet joints. Medial branch blocks are nerve-blocking injections administered to the nerves associated with the facet joints. These procedures are minimally invasive and are associated with significant pain relief for many patients. The effects of nerve blocks may last from a number of weeks to a month or more. If this treatment is appropriate for you, the appropriate schedule of procedures can be worked out between you and a pain specialist based on your response to the initial nerve block. The various types of nerve blocks are associated with some risks, however. Local anesthetics are associated with side effects such as chest numbness and discomfort. Serious side effects, such as heart rate irregularities, may also occur. Steroid administration is also associated with risks, such as immune system dysfunction, gastrointestinal distress, and mood changes.

If these interventions fail, a patient may consider a more permanent strategy for relief from spondylosis-related pain. Spinal cord stimulators (SCS) are medical devices designed for long-term effective pain relief. They are implanted surgically near points in the spinal cord subject to damage from conditions such as spondylosis. The implants emit a mild electrical impulse when activated by the patient, which modulate or correct the excessive pain signals that travel from damaged spinal tissue to the brain. At first, temporary stimulators may be implanted to assess the patient’s response. This implant may be in place for some days, as the patient tests its ability to inhibit pain. If the patient feels the trial is effective, a permanent device may be implanted. The stimulator is located within or near the spinal bones affected by spondylosis, and connected to a hand-held control device via leads protruding through the skin. With this, the patient can activate the impulses in response to the onset of pain. Spinal cord stimulation is associated with durable, long-lasting pain relief.
Spinal cord stimulation is in widespread use, and is safe in the vast majority of cases. However, it is associated with some risks and side effects. These include infection in the skin and tissues through which implants are placed, and through which the device’s leads are connected to the external controller. These leads may also cause scar tissue to form around them in some rare cases. This is associated with the increased risk of inflammation and chronic pain in the surrounding tissues. Bleeding and cerebrospinal fluid leakage from the surgical incisions made is also possible. Spinal cord stimulation may be ineffective if it does not line up accurately enough with the areas of the spinal cord it is meant to treat. Inaccurate device placement may also result in nerve damage, which may cause pain, motor control problems, or numbness depending on the regions of the spine affected.
Conclusion
Spondylosis is a condition in which one or more of the bones of the spine (vertebrae) are subject to degeneration. This may result in numbness, motor problems, or chronic pain. It is commonly linked to arthritis (an autoimmune condition that targets joints), but may also result from wear and tear over time. Spondylosis may contribute to other serious spinal conditions such as stenosis, which are also associated with chronic pain. This condition may be treated with conventional medications such as muscle relaxants and non-steroidal anti-inflammatory drugs. If these prove ineffective, a pain specialist may recommend injections of medications that inhibit pain or inflammation, administered to spinal nerves affected by spondylosis. Patients with pain that is resistant even to this treatment may consider more long-term solutions such as spinal cord stimulation.
References
- Omidi-Kashani F, Hasankhani EG, Ashjazadeh A. Lumbar spinal stenosis: who should be fused? An updated review. Asian Spine J. 2014;8(4):521-530.
- Klessinger S, Freund W, Karpel-Massler G, Halatsch M-E. Response to transforaminal injection of steroids and correlation to mri findings in patients with cervical radicular pain or radiculopathy due to disc herniation or spondylosis. Pain Med. 2014;15(6):929-937.
- Schairer WW, Carrer A, Lu M, Hu SS. The Increased Prevalence of Cervical Spondylosis in Patients with Adult Thoracolumbar Spinal Deformity. J Spinal Disord Tech. 2014.
- Di Z, Jiang S, Lin X-M, Fu W-B. [The short-term and long-term effects on neck pain caused by cervical spondylosis treated with combination of acupuncture and moxibustion with seed-sized moxa cone]. Zhongguo Zhen Jiu. 2014;34(4):325-328.
- Kalsi-Ryan S, Karadimas SK, Fehlings MG. Cervical spondylotic myelopathy: the clinical phenomenon and the current pathobiology of an increasingly prevalent and devastating disorder. Neuroscientist 2013;19(4):409-421.
- Parker SL, Godil SS, Mendenhall SK, Zuckerman SL, Shau DN, McGirt MJ. Two-year comprehensive medical management of degenerative lumbar spine disease (lumbar spondylolisthesis, stenosis, or disc herniation): a value analysis of cost, pain, disability, and quality of life: clinical article. J Neurosurg Spine. 2014;21(2):143-149.
- McAuley J, Farah N, van Gröningen R, Green C. A questionnaire-based study on patients’ experiences with rechargeable implanted programmable generators for spinal cord stimulation to treat chronic lumbar spondylosis pain. Neuromodulation. 2013;16(2):142-146.