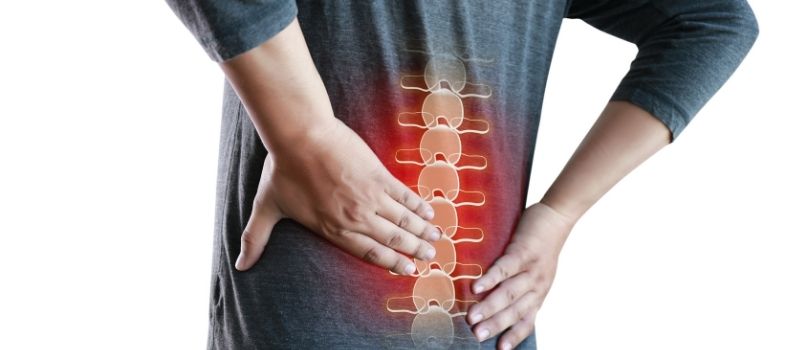
Postlaminectomy Syndrome, also known as failed back surgery syndrome, is a condition that occurs in some individuals who have undergone spinal surgery. Despite the initial relief provided by the surgery, these individuals experience persistent or recurring pain in the back and legs. It is important to understand the causes, symptoms, and treatment options available for Postlaminectomy Syndrome in order to effectively manage this condition.
What is Postlaminectomy Syndrome?
Postlaminectomy Syndrome refers to the symptoms that develop after a laminectomy or other spinal surgery. A laminectomy involves removing a portion of the bony arch (lamina) of a vertebra to relieve pressure on the spinal cord or nerves. While this procedure can alleviate pain caused by spinal stenosis or herniated discs, it is not always successful in providing long-term relief.
Defining Postlaminectomy Syndrome
Postlaminectomy Syndrome is characterized by persistent or recurring pain in the back and/or legs following spinal surgery. This pain can be dull, aching, or sharp in nature. It may also be accompanied by other symptoms such as numbness, tingling, weakness, or reduced mobility.
Common Misconceptions about Postlaminectomy Syndrome
There are several misconceptions surrounding Postlaminectomy Syndrome that can hinder understanding and treatment. One common misconception is that the pain experienced after surgery is a normal part of the healing process. However, persistent or worsening pain should not be ignored and should be evaluated by a healthcare professional.
Another misconception is that Postlaminectomy Syndrome only occurs if the initial surgery was unsuccessful. In reality, this condition can develop even if the surgery was technically successful in relieving the initial source of pain.
It is important to note that the development of Postlaminectomy Syndrome is not necessarily indicative of a medical error or negligence. The human body is complex, and individual responses to surgery can vary greatly. Factors such as pre-existing conditions, the extent of the initial spinal damage, and the body’s healing process can all contribute to the development of this syndrome.
Research suggests that the exact cause of Postlaminectomy Syndrome is multifactorial. It is believed to involve a combination of mechanical, chemical, and neurophysiological factors. The surgical procedure itself can cause tissue trauma, leading to inflammation and nerve irritation. Additionally, scar tissue formation around the surgical site can contribute to ongoing pain and discomfort.
Psychological factors can also play a role in the development and persistence of Postlaminectomy Syndrome. Chronic pain can have a significant impact on a person’s mental and emotional well-being, leading to anxiety, depression, and a decreased quality of life. Addressing these psychological factors through therapy and support can be an important aspect of managing the syndrome.
Treatment options for Postlaminectomy Syndrome vary depending on the individual and the severity of symptoms. Conservative approaches may include physical therapy, pain medications, and lifestyle modifications. In some cases, additional surgical interventions may be necessary to address the underlying cause of the ongoing pain.
It is crucial for individuals experiencing symptoms of Postlaminectomy Syndrome to work closely with their healthcare team to develop a personalized treatment plan. Open communication, regular follow-up appointments, and a collaborative approach can help optimize outcomes and improve quality of life for those affected by this condition.
The Causes of Postlaminectomy Syndrome
Postlaminectomy Syndrome, also known as failed back surgery syndrome, is a condition that can occur after spinal surgery. It is characterized by persistent pain and discomfort in the back or legs, despite the initial surgery. The causes of this syndrome can be multifactorial, involving both surgical and non-surgical factors.
Surgical Factors
One potential cause of Postlaminectomy Syndrome is scar tissue formation at the surgical site. When the body heals after surgery, it naturally forms scar tissue. However, in some cases, excessive scar tissue can develop, leading to compression of nearby nerves. This compression can result in chronic pain and discomfort.
In addition to scar tissue formation, hardware failure can also contribute to the development of Postlaminectomy Syndrome. Surgical procedures often involve the use of implants, such as screws, rods, or cages, to stabilize the spine. If these implants fail or become dislodged, it can lead to instability and subsequent pain.
Complications during the surgery can also play a role in the development of this condition. Infections, although rare, can occur after spinal surgery and cause inflammation and pain. Nerve damage during the surgery can result in ongoing neurological symptoms, such as numbness, tingling, or weakness.
Non-Surgical Factors
While surgical factors are important contributors to Postlaminectomy Syndrome, non-surgical factors can also play a significant role in its development. These factors include preexisting spinal conditions that may not have been fully addressed during the initial surgery.
For example, degenerative disc disease, a condition characterized by the breakdown of spinal discs, can lead to ongoing pain even after surgery. If the degenerated discs were not adequately treated, the symptoms may persist and contribute to Postlaminectomy Syndrome.
Arthritis, another common spinal condition, can also be a non-surgical factor in the development of this syndrome. Inflammation and joint degeneration associated with arthritis can cause ongoing pain and discomfort, even after surgical intervention.
Furthermore, lifestyle factors can also contribute to the development of ongoing pain. Obesity, for instance, can put additional stress on the spine, leading to increased pain and reduced surgical outcomes. Smoking, known to impair healing and reduce blood flow, can negatively impact the recovery process and contribute to the persistence of symptoms.
Lastly, poor postoperative rehabilitation can hinder the healing process and contribute to the development of ongoing pain. Inadequate physical therapy or failure to follow postoperative instructions can result in muscle weakness, poor spinal alignment, and increased pain.
In conclusion, Postlaminectomy Syndrome can have various causes, both surgical and non-surgical. Understanding these factors is crucial for healthcare professionals to provide appropriate treatment and management strategies for individuals experiencing this challenging condition.
Recognizing the Symptoms of Postlaminectomy Syndrome
Postlaminectomy Syndrome is a condition that can occur after spinal surgery, specifically after laminectomy, which is the removal of the lamina, a part of the vertebral bone. It is important to recognize the symptoms of Postlaminectomy Syndrome in order to seek appropriate medical care and treatment.
After undergoing spinal surgery, it is common for patients to experience some degree of pain and discomfort during the recovery period. However, if the pain persists or worsens over time, it may be a sign of Postlaminectomy Syndrome.
Physical Symptoms
The physical symptoms of Postlaminectomy Syndrome can vary from person to person. Common physical symptoms include persistent or recurring pain in the back and/or legs, limited mobility, muscle weakness, and sensory abnormalities such as numbness or tingling.
The pain experienced in Postlaminectomy Syndrome can be localized to the surgical site or radiate to other areas of the body. It may be described as sharp, shooting, burning, or throbbing. The intensity of the pain can range from mild to severe, and it may be aggravated by certain movements or activities.
In addition to pain, individuals with Postlaminectomy Syndrome may also experience limited mobility. This can make it difficult to perform everyday tasks and activities, such as walking, bending, or lifting objects. Muscle weakness is another common physical symptom, which can further contribute to reduced mobility and functional limitations.
Sensory abnormalities, such as numbness or tingling, are also frequently reported in individuals with Postlaminectomy Syndrome. These sensations may occur in the back, legs, or other parts of the body, and they can be constant or intermittent.
Psychological Symptoms
In addition to physical symptoms, Postlaminectomy Syndrome can also cause psychological symptoms. Living with chronic pain can lead to emotional distress, anxiety, depression, and reduced quality of life. It is important for healthcare providers to address these psychological symptoms along with the physical symptoms to provide holistic care.
Chronic pain can have a significant impact on a person’s mental well-being. It can lead to feelings of frustration, helplessness, and hopelessness. The constant presence of pain can also disrupt sleep patterns, leading to fatigue and irritability.
Anxiety is another common psychological symptom experienced by individuals with Postlaminectomy Syndrome. The fear of exacerbating the pain or causing further damage can result in avoidance of certain activities or social situations. This can lead to social isolation and a decreased sense of self-worth.
Depression is also prevalent in individuals with Postlaminectomy Syndrome. The chronic pain and physical limitations can make it challenging to engage in activities that were once enjoyable, leading to a loss of interest and pleasure. Feelings of sadness, emptiness, and a lack of motivation may accompany this condition.
Reduced quality of life is a significant concern for individuals with Postlaminectomy Syndrome. The combination of physical and psychological symptoms can impact various aspects of daily life, including work, relationships, and overall well-being.
In conclusion, recognizing the symptoms of Postlaminectomy Syndrome is crucial for early intervention and appropriate management. The physical symptoms, such as persistent pain, limited mobility, muscle weakness, and sensory abnormalities, should not be overlooked. Additionally, the psychological symptoms, including emotional distress, anxiety, depression, and reduced quality of life, should be addressed to provide comprehensive care for individuals with Postlaminectomy Syndrome.
Diagnostic Procedures for Postlaminectomy Syndrome
Accurate diagnosis plays a crucial role in determining the most appropriate treatment options for Postlaminectomy Syndrome.
Medical History and Physical Examination
During the diagnostic process, healthcare providers will take a detailed medical history and perform a thorough physical examination. This includes assessing the range of motion, muscle strength, and reflexes, as well as evaluating for any signs of infection or neurological deficits.
Imaging Tests
In addition to the physical examination, imaging tests such as X-rays, magnetic resonance imaging (MRI), or computed tomography (CT) scans may be ordered to visualize the spinal structures and identify any potential sources of pain or complications from the previous surgery.
Treatment Options for Postlaminectomy Syndrome
There are various treatment options available to manage the symptoms of Postlaminectomy Syndrome.
Non-Invasive Treatments
Non-invasive treatments are often the first line of management for Postlaminectomy Syndrome. These may include physical therapy, chiropractic care, acupuncture, pain medication, or the use of assistive devices such as back braces or canes to improve mobility and reduce pain.
Psychological interventions like cognitive-behavioral therapy can also be beneficial in addressing the psychological symptoms associated with chronic pain.
Surgical Treatments
In some cases, surgical intervention may be necessary to address the underlying cause of Postlaminectomy Syndrome. Revision surgery may be performed to remove scar tissue, address hardware complications, or further decompress nerves that were not successfully relieved during the initial surgery.
It is important for individuals considering surgery to have a thorough discussion with their healthcare provider to weigh the benefits and risks of the procedure.
In conclusion, understanding the causes, symptoms, and treatment options for Postlaminectomy Syndrome is crucial in effectively managing this condition. Postlaminectomy Syndrome can occur even after a technically successful surgery, and its symptoms can have a significant impact on an individual’s physical and psychological well-being. Working closely with healthcare providers to accurately diagnose and implement an appropriate treatment plan can help individuals find relief from the persistent pain and improve their quality of life.