What are Trigger Point Injections?
Trigger point injections (TPI) are a simple procedure widely performed to relieve myofascial pain[1]. It involves injection of medications into trigger points, or knots that form when muscles do not relax.
A myofascial trigger point, or knot, is a hyperirritable spot, usually located within a taut band of skeletal muscle, which feels painful upon compression and can give rise to characteristic pain, motor dysfunction, and autonomic phenomena[2]. Trigger points produce local and referred pain and often accompany chronic musculoskeletal disorders[3].
Knots can be felt as nodules or bands in the muscle. Stimulation of a knot may elicit a twitch response and pain, which may radiate in a distribution consistent with the affected muscle.
Conditions Treated with Trigger Point Injections
A pain syndrome commonly treated with trigger point injections is fibromyalgia, a chronic condition involving widespread pain, fatigue, sleep abnormalities, and often distress. The authors of a controlled study in fibromyalgia patients concluded the overall spontaneous fibromyalgia pain pattern can be reproduced by mechanical stimulation of active trigger points located in different muscles, suggesting fibromyalgia pain arises largely from muscle pain and spasm[13]. According to another study in fibromyalgia patients, tender points located at examination sites specified by American College of Rheumatology criteria are almost universally myofascial trigger points[14]. And two recent reviews concluded local extinction of trigger points in patients with fibromyalgia produces significant relief of fibromyalgia pain[15], and improves range of motion[16].
Trigger point injections are also used to treat chronic pelvic pain syndrome, which involves lower urinary tract symptoms, chronic pelvic pain, sexual dysfunction, interstitial cystitis, painful bladder syndrome in women, and chronic prostatitis in men[17]. There may be an association between myofascial trigger points and reported painful sites in individuals with this syndrome[18], and concentrating therapy on clusters of trigger points inside and outside the pelvic floor may help relieve symptoms[19]. A 2011 Stanford University study found men with chronic pelvic pain refractory to traditional treatment benefitted from intensive myofascial trigger point therapy and concomitant paradoxical relaxation training[20]. And another study found application of the trigger point release/paradoxical relaxation training protocol in men was associated with significant improvement in pelvic pain, urinary symptoms, libido, ejaculatory pain, and erectile and ejaculatory dysfunction[21].
Patients with chronic headaches sometimes receive trigger point injections to assist in controlling the pain. One theory is that referred pain from trigger points in head, neck, and shoulder muscles produces head pain[22],[23]. According to a survey conducted by the International Headache Society, the most common indications for the use of TPIs in headache patients are chronic tension-type headache and chronic migraine[24]. Further, a 2008 study in chronic cluster headache patients found trigger point injections were associated with significant improvement in 7 of 8 chronic cluster headache patients[25].
Additionally, trigger point injections are being investigated as a treatment for whiplash, an acute condition involving neck pain after sudden backwards and forwards motion, as may occur in an automobile accident. According to the authors of a preliminary study, trigger points are considered a primary cause of pain in whiplash injured patients[26]. A controlled study in 17 whiplash patients with chronic and intractable neck pain showed several beneficial effects in individuals who received TPI[27]. The study subjects were evaluated for cervical range of motion, pressure pain thresholds, sensitivity to light (photophobia) and perception of pain using a visual analog scale (VAS) before and after injections. Immediate (within 1 minute) alterations in cervical range of motion and pressure pain thresholds were observed following an average of 3.8 injections with 1% lidocaine into carefully identified trigger points. Cervical range of motion increased by an average of 49%, and pressure pain thresholds were found increased by 68%, 78%, and 64% over three different affected body areas, respectively. Among 11 subjects with photophobia, only 2 remained sensitive to light after the TPIs, and average VAS dropped by 57%.
Trigger Point Injections Procedure
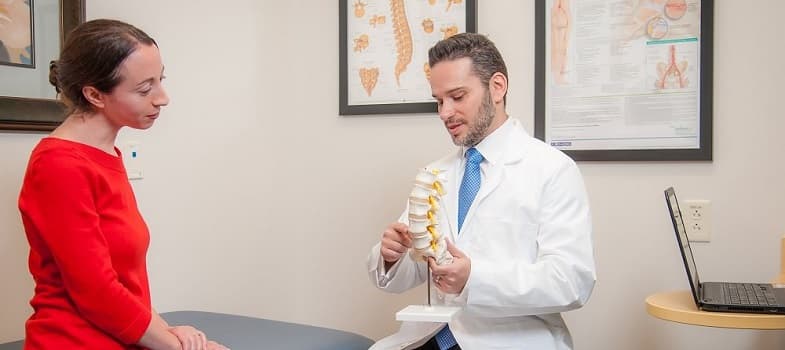
In a trigger point injections procedure, a health care professional exerts gentle pressure upon a trigger point to observe muscle twitch and evaluate the patient’s pain. This may be accomplished using a hand or a special device. The purpose of this examination is to allow the provider to identify muscles causing pain that could benefit from injections.
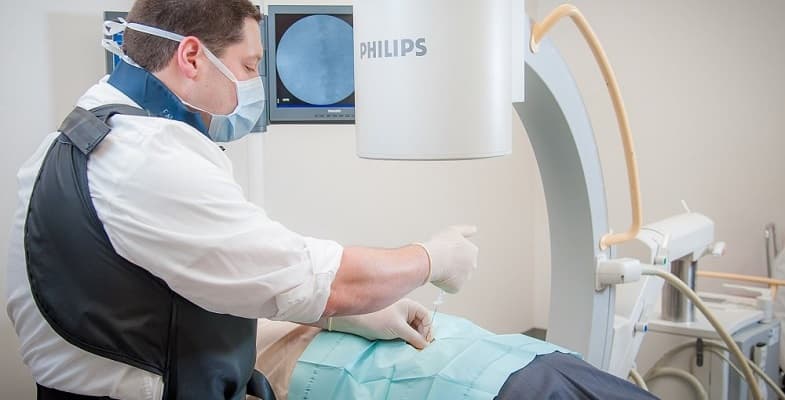
When the painful area has been identified, the practitioner uses a small needle to inject medications into the trigger point. Common treatment sites include the arms, legs, low back, and neck. Typically, TPI medications include a local anesthetic (painkiller) and a synthetic steroid (corticosteroid). These medications work in concert to lower inflammation and disperse the trigger point. Injection of botulinum toxin A (botox) into trigger points has also been reported as effective[28],[29],[30]. In some cases, no medications are injected; this is called a dry needling technique and is effective in certain patients. For example, a 2010 study of dry needling in elite volleyball players with painful shoulder injuries produced significant improvements in range of movement, strength and pain[31]. Normally, a brief course of TPIs results in sustained pain relief. The injections are given in the doctor’s office and take only a few minutes to administer. Several sites may be injected in one session.
Trigger point injections are a preferred means of treating pain disorders and other painful conditions because it is a minimally invasive treatment. Less invasive procedures provide compelling advantages over more invasive procedures such as open surgery. These advantages include quicker recovery time, lower risk of infection and other complications, minimal scarring, and outpatient setting.
Since myofascial pain conditions can profoundly affect quality of life, TPI provides an effective, quick, safe and minimally invasive solution to pain management in certain patients.
As with any medical procedure, trigger point injections are associated with various risks. A review of medical literature for documented complications associated with interventional pain management, specifically those associated with joint, tendon, and muscle injections, found the most common complication appears to be infection, including spondylodiscitis, septic arthritis, epidural abscess, necrotizing fascitis, and osteomyelitis.[32]. Other reported complications include spinal cord injury and peripheral nerve injuries, pneumothorax, air embolism, pain or swelling at the site of injection, chemical meningism, and tendon and fascial ruptures. In addition, one case study reported a patient who received TPI developed myositis ossificans[33], an inflammatory condition that causes calcification of soft tissues, or abnormal bone formation within muscle, tendons, and ligaments. As noted by the authors of the review, many of these complications may be preventable by choosing an experienced practitioner who adheres strictly to aseptic techniques, has refined the procedure, and who is exceptionally familiar with the relevant anatomies.
Trigger points can cause recurrent pain and inactivity, and can significantly lower quality of life. Fortunately, the doctors at Wake Spine & Pain Specialists understand the burden of living with pain and are highly experienced in the treatment of pain syndromes. Schedule a consultation today to learn about the numerous interventions available to help manage chronic pain.
At Wake Spine & Pain Specialists our goal is to relieve your pain and improve function to increase your quality of life.
Give us a call today at (919)-787-7246.[/color-box]
References
- Shin SJ, & Kang SS. (2011). Myositis ossificans of the elbow after a trigger point injection. Clin Orthop Surg., 3(1), 81-5.
- Lavelle ED, Lavelle W, & Smith HS. (2007). Myofascial trigger points. Anesthesiol Clin., 25(4), 841-51, vii-iii.
- Alvarez DJ, & Rockwell PG. (2002). Trigger points: diagnosis and management. Am Fam Physician., 65(4), 653-60.
- Malanga GA, & Cruz Colon EJ. (2010). Myofascial low back pain: a review. Phys Med Rehabil Clin N Am., 21(4), 711-24.
- Venâncio Rde A, Alencar FG, Zamperini C. (2008). Different substances and dry-needling injections in patients with myofascial pain and headaches. Cranio., 26(2), 96-103.
- Corujeira Rivera MC, Carregal Rañó A, Diz Gómez JC, Mayo Moldes M, Prieto Requeijo P, & Areán González I. (2010). [Evaluation of 2 invasive techniques for treating myofascial pain].[Article in Spanish]. Rev Esp Anestesiol Reanim., 57(2), 86-90.
- Venancio Rde A, Alencar FG Jr, & Zamperini C. (2009). Botulinum toxin, lidocaine, and dry-needling injections in patients with myofascial pain and headaches. Cranio., 27(1), 46-53.
- Graboski CL, Gray DS, & Burnham RS. (2005). Botulinum toxin A versus bupivacaine trigger point injections for the treatment of myofascial pain syndrome: a randomised double blind crossover study. Pain., 118(1-2), 170-5.
- Esenyel M, Caglar N, & Aldemir T. (2000). Treatment of myofascial pain. Am J Phys Med Rehabil., 79(1), 48-52.
- Bubnov RV. (2010). The use of trigger point “dry” needling under ultrasound guidance for the treatment of myofascial pain (technological innovation and literature review). Lik Sprava., (5-6), 56-64.
- Unalan H, Majlesi J, Aydin FY, & Palamar D. (2011). Comparison of high-power pain threshold ultrasound therapy with local injection in the treatment of active myofascial trigger points of the upper trapezius muscle. Arch Phys Med Rehabil., 92(4), 657-62.
- Bron C, de Gast A, Dommerholt J, Stegenga B, Wensing M, Oostendorp RA. (2011). Treatment of myofascial trigger points in patients with chronic shoulder pain: a randomized, controlled trial. BMC Med., 24, 9:8.
- Ge HY, Wang Y, Fernández-de-Las-Peñas C, Graven-Nielsen T, Danneskiold-Samsøe B, & Arendt-Nielsen L. Reproduction of overall spontaneous pain pattern by manual stimulation of active myofascial trigger points in fibromyalgia patients. Arthritis Res Ther., 13(2), R48.
- Gerwin RD. (2011). Fibromyalgia tender points at examination sites specified by the American College of Rheumatology criteria are almost universally myofascial trigger points. Curr Pain Headache Rep., 15(1), 1-3.
- Giamberardino MA, Affaitati G, Fabrizio A, & Costantini R. (2011). Effects of Treatment of Myofascial Trigger Points on the Pain of Fibromyalgia. Curr Pain Headache Rep., 2011 May 5. [Epub ahead of print]
- Borg-Stein J, & Stein J. (1996). Trigger points and tender points: one and the same? Does injection treatment help? Rheum Dis Clin North Am., 22(2), 305-22.
- Wehbe SA, Fariello JY, Whitmore K. (2010). Minimally invasive therapies for chronic pelvic pain syndrome. Curr Urol Rep., 11(4), 276-85.
- Labat JJ, Guerineau M, Delavierre D, Sibert L, & Rigaud J. (2010). [Symptomatic approach to musculoskeletal dysfunction and chronic pelvic and perineal pain]. [Article in French]. Prog Urol., 20(12), 982-9.
- Anderson RU, Sawyer T, Wise D, Morey A, & Nathanson BH. (2009). Painful myofascial trigger points and pain sites in men with chronic prostatitis/chronic pelvic pain syndrome. J Urol., 182(6), 2753-8.
- Anderson RU, Wise D, Sawyer T, Glowe P, Orenberg EK. (2011). 6-day intensive treatment protocol for refractory chronic prostatitis/chronic pelvic pain syndrome using myofascial release and paradoxical relaxation training. J Urol. 185(4), 1294-9.
- Anderson RU, Wise D, Sawyer T, & Chan CA. (2006). Sexual dysfunction in men with chronic prostatitis/chronic pelvic pain syndrome: improvement after trigger point release and paradoxical relaxation training. J Urol., 176(4 Pt 1), 1534-8; discussion 1538-9.
- Fernández-de-las-Peñas C, Fernández-Mayoralas DM, Ortega-Santiago R, Ambite-Quesada S, Palacios-Ceña D, Pareja JA. (2011). Referred pain from myofascial trigger points in head and neck-shoulder muscles reproduces head pain features in children with chronic tension type headache.J Headache Pain., 12(1), 35-43.
- Fernández-de-Las-Peñas C, Ge HY, Alonso-Blanco C, González-Iglesias J, & Arendt-Nielsen L. (2010). Referred pain areas of active myofascial trigger points in head, neck, and shoulder muscles, in chronic tension type headache. J Bodyw Mov Ther., 14(4), 391-6.
- Blumenfeld A, Ashkenazi A, Grosberg B, Napchan U, Narouze S, Nett B, DePalma T, Rosenthal B, Tepper S, & Lipton RB. (2010). Patterns of use of peripheral nerve blocks and trigger point injections among headache practitioners in the USA: Results of the American Headache Society Interventional Procedure Survey (AHS-IPS). Headache., 50(6), 937-42.
- Calandre EP, Hidalgo J, Garcia-Leiva JM, Rico-Villademoros F, & Delgado-Rodriguez A. (2008). Myofascial trigger points in cluster headache patients: a case series. Head Face Med., 4, 32.
- Tough EA, White AR, Richards SH, & Campbell JL. (2010). Myofascial trigger point needling for whiplash associated pain–a feasibility study. Man Ther., 15(6), 529-35.
- Freeman MD, Nystrom A, & Centeno C. (2009). Chronic whiplash and central sensitization; an evaluation of the role of a myofascial trigger points in pain modulation. J Brachial Plex Peripher Nerve Inj., 4, 2.
- Cheshire WP, Abashian SW, Mann JD. (1994). Botulinum toxin in the treatment of myofascial pain syndrome. Pain., 59(1), 65-9.
- Venancio Rde A, Alencar FG Jr, Zamperini C. (2009). Botulinum toxin, lidocaine, and dry-needling injections in patients with myofascial pain and headaches. Cranio., 27(1), 46-53.
- Harden RN, Cottrill J, Gagnon CM, Smitherman TA, Weinland SR, Tann B, Joseph P, Lee TS, & Houle TT. (2008). Botulinum toxin a in the treatment of chronic tension-type headache with cervical myofascial trigger points: a randomized, double-blind, placebo-controlled pilot study.Headache., 49(5), 732-43.
- Osborne NJ, & Gatt IT. (2010). Management of shoulder injuries using dry needling in elite volleyball players. Acupunct Med., 28(1), 42-5.
- Cheng J, & Abdi S. (2007). Complications of joint, tendon and muscle injections. Tech Reg Anesth Pain Manag., 11(3), 141-147.
- Shin SJ, & Kang SS. (2011). Myositis ossificans of the elbow after a trigger point injection. Clin Orthop Surg., 3(1), 81-5.